Hidradenitis suppurativa, sometimes called acne inversa, affects millions of people worldwide, and up to 200,000 people in the United States are diagnosed with moderate to severe cases each year. HS is a very complex disease that can often go undiagnosed for log periods of time, even years. This seems scary, and it can be, but the providers at Pine Belt Dermatology can help you obtain accurate information about HS and provide the best treatment options available.
Hidradenitis suppurativa is a chronic, long lasting, inflammatory skin condition that can be caused by malfunctions in the body’s immune system. This disease can often start with a bump on your inner thigh and can sometimes even be mistaken for a pimple on your inner thigh or in your armpit. The difference between regular pimples and HS is that the pimple-like bumps that appear typically surface in areas that every-day acne would not typically surface. These bumps that can be mistaken for pimples will then progress to painful abscesses that may eventually rupture. If you have HS, or think you might have it, it is extremely important that you come to see one of our providers here at Pine Belt Dermatology & Skin Cancer.
As I alluded to when I mentioned the importance of obtaining accurate information regarding the skin condition, there are a lot of myths that are floating around regarding hidradenitis suppurativa and I want to address some of them in this blog.
Some of the myths – which are not true- include:
- HS is a sexually transmitted disease
- HS is caused by poor personal hygiene habits
- HS can be contagious
- You are responsible for developing the disease.
More information regarding the symptoms of hidradenitis suppurativa:
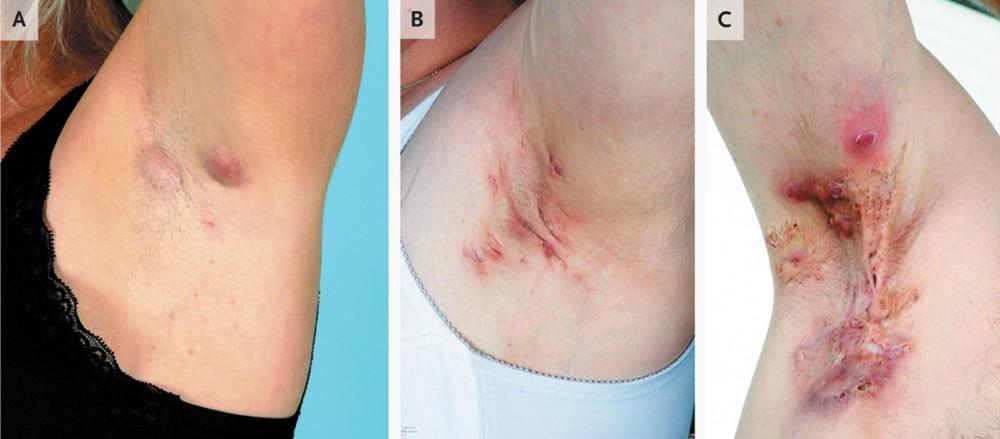
The bumps that initially appear with this disease seem benign and innocent, which can make it difficult to initially recognize as HS. Hidradenitis suppurativa bumps can be mistaken for a few different conditions: acne, boils, folliculitis, and deep-acne cysts or blackheads. However, these bumps can manifest over time to become painful abscesses that leak foul-smelling, bloodstained pus. There have been instances where the symptoms appear and then seemingly subside, but these can flare up again within weeks, months, or years later. It is important if you have symptoms you believe to be that of HS that you schedule a consultation with myself or one of my colleagues. The recurrence of HS can lead to scarring in the affected areas where it continues to come back. As the deep bumps heal, some people develop tunnel-like tracts under their skin. As the skin continues to heal and scar, the scars thicken. When thick scars form in the underarm, moving the arm can be difficult. Thick scars in the groin area can make walking difficult. This is why we stress coming to see us if you experience any of the symptoms described. Pine Belt Dermatology can help determine the severity of your case of hidradenitis suppurativa and then tailor treatment options to you specifically, and early treatment will help prevent the condition from worsening.
Severities of HS:
- Mild HS usually is a single abscess, or sometimes a couple abscesses, without draining wounds.
- Moderate HS is typically when these single or few abscesses become widespread in an area (i.e the armpits).
- Severe HS typically means there are many abscesses that are clustered and cover a large area of the body.
Symptoms of worsening hidradenitis suppurativa:
- Painful, deep breakouts that heal and reappear.
- Breakouts that rupture and leave a foul-smelling odor.
- Scars that form in areas of recurrence.
- Scars that become extremely thick.
- Skin that becomes/appears spongey due to the tracts of scarring that form deep within the skin.
- Serious infections.
- In rare instances, skin cancer can develop in affected areas.
Though exact causes of hidradenitis suppurativa are still no entirely clear, there is some solid data surround the risk factors, who gets HS, and how it can affect different groups. Some of the data for different demographics are discussed a little further in depth below:
- Age: hidradenitis suppurativa typically develops around puberty and also commonly develops in young adults in their early 20s, but it can develop at any age. One interesting fact is that developing HS in ages later than 55 is quite rare.
- Sex: HS, for reasons that are unclear, occurs more frequently in women. In fact, women are three times more likely to develop hidradenitis suppurativa than men.
- Family/Medical History seems to play a part in the risks associated with developing HS. Research shows that there can be a genetic component associated with development of the disease. One statistic to note is that more than 1/3 of the people diagnosed with HS have a family member also living with the disease. Medical history of the individual also seems to play a role in the associated risk. HS can affect all body types, however, many people with hidradenitis suppurativa have had a history of being overweight and having had acne. It should be noted that these previous conditions do not guarantee that you will develop HS later in life.
You may notice signs and symptoms of the disease, including swelling and abscesses. Symptoms like pain of the lesions can significantly impact your day-to-day mobility. It can make something as simple as moving your arms difficult. As stated above, if you think you have the symptoms schedule an appointment with us today.
What areas of the body does the disease affect?
We’ve discussed previously that the disease varies men and women, and the same is true for the areas that are affected.
Women:
- Underarms
- Under the breasts
- Buttocks
- Groin area
- Inner thighs
Men:
- Ears
- Back of the neck
- Underarms
- Buttocks
- Groin area
- Inner thighs
Tips for Reducing Frequency of Flare-Ups:
- Lose weight to lessen HS — or even clear your skin. If you are overweight, losing weight may be the most effective way to control HS. It may even be more effective than treatment. Dermatologists have found that when patients who have HS lose weight, they have fewer flare-ups. Losing just 10% of your body weight can make a difference. Losing weight has additional benefits for people who have HS. Findings from one medical study showed that having HS increases the risk for developing other health problems, including heart disease and diabetes. HS also increases the risk of having a stroke. Losing weight and eating a well-balanced diet on most days can reduce these risks.
- Quit smoking to reduce HS flare-ups. Quitting smoking can help you live a longer, healthier life. It also can reduce HS flare-ups and decrease the severity of HS.
- Stop shaving where you have breakouts. Shaving can irritate the skin. If you want to remove the hair, ask your dermatologist what you can safely use to remove the hair.
- Wear loose-fitting clothes to reduce friction. Tight waistbands and form-fitting clothes tend to rub against your skin, causing HS to flare. Wearing loose-fitting clothes, including underwear, can help.
- Keep your skin cool. Overheating and sweating can cause HS to flare. If you need a product that can help reduce sweating, such as an antiperspirant, ask your dermatologist for a recommendation. Some antiperspirants are too harsh for skin affected by HS.
Because HS is not very well known, people who have the disease have a tendency to be given false information and also tend to feel as if they are alone in their struggle. It is important to know that there are others out there that can relate to your day-to-day struggle, and that treatment options are available. I cannot stress the importance of seeing a PBD provider for the disease either. We specialize in diagnosing and treating inflammatory skin conditions including that of HS. Inflammatory skin conditions can be misdiagnosed by other types of doctors, as is often the case with skin conditions.