Lupus is an extremely tricky disease to diagnose because it can often times be confused with a myriad of other conditions. In fact, when it was first discovered in the thirteenth century, the lesions on the face of patients resembled that of patients who had been bitten by a wolf. Hence the condition was branded the name “lupus” (Latin for wolf). Presently, just as it perplexed physicians who treated the condition centuries ago, it is still often difficult to diagnose despite our more advanced understanding of the disease. Providers at Pine Belt Dermatology & Skin Cancer Center can assist in determining whether or not you have Lupus. This blog is intended to be an overview of the disease and how we may be able to play a vital role in catching the disease and maintaining it.
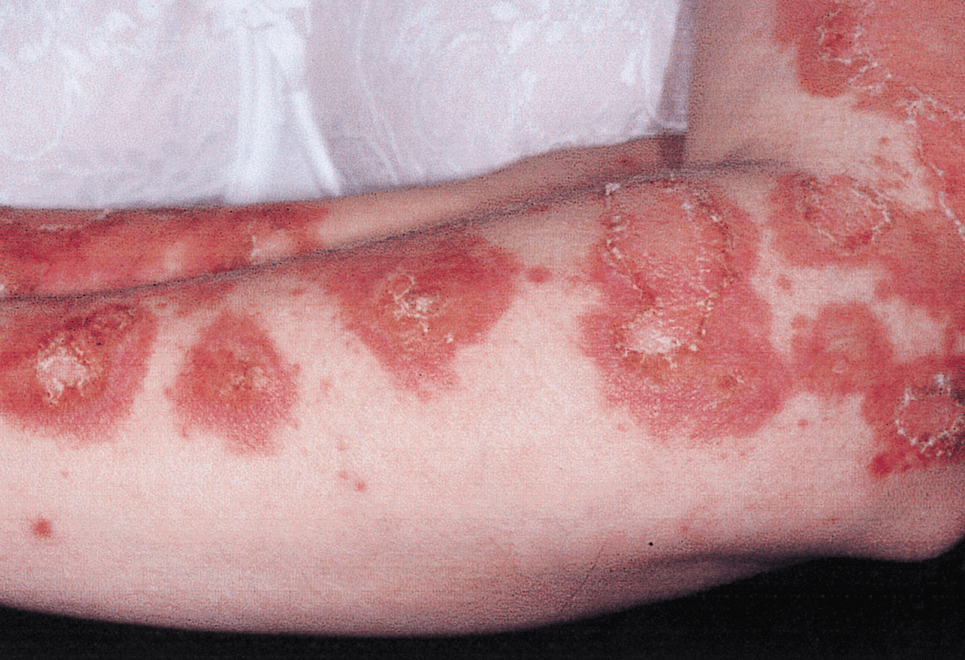
Lupus is a chronic auto immune disease that can cause your body to attack a number of organ systems such as the skin, brain, heart, lungs, joints, kidneys, and blood cells. As previously mentioned, Lupus is a difficult disease to diagnose because it mimics a vast number of other conditions. Dermatology plays a pivotal role in diagnosing Lupus because the most distinctive symptom of Lupus is the butterfly rash. This is a facial rash that spreads across the nose and cheeks in the shape of a butterfly. When Lupus affects the skin, it often causes rashes or sores. Depending on the type of Lupus, these rashes and sores can vary. Some Lupus rashes can damage the blood vessels near the surface of the skin and these damages can become visible. Another condition that can occur is a phenomenon called “Raynaud’s phenomenon”. This condition restricts blood flow which causes the tips of the fingers or toes to turn white, red, or even blue in response to cold weather or stress. In some cases, patients with this condition can also experience numbness, tingling, or pain when in cold weather or under stress. Lupus can also cause hair loss in some patients. This condition is called “lupus hair” and it often occurs in patients who have systemic lupus erythematosus (SLE), which is the most common type of Lupus. In many cases, when the Lupus flare subsides the hair will start to grow back. Patients who have discoid lupus erythematosus (DLE), which is a type of lupus that primarily affects the skin, can sometimes experience permanent hair loss from the flare ups. When the rash appears on the scalp it can cause the scalp to scar once it heals and when that happens it will result in permanent hair loss. Other features in the skin that can indicate Lupus include:
- Sores in the mouth or nose.
- Knots and sores, especially on the lower legs.
- Blue/purplish lacelike pattern on the skin that is usually on the legs.
- Flare-ups that can look like sunburn (or Rosacea).
- Reddish-purple spots or bumps that appear on the lower legs.
- A rash that spreads across the back.
- Thick and scaly patches of skin on the face.
Lupus affecting the skin is termed cutaneous Lupus. Most individuals who have this variation of Lupus only experience the symptoms affecting the skin. Of course, each case is different and so it is vital to see one of our providers to rule out other possible conditions. Some suspected cases of cutaneous Lupus may turn out to just be severely inflamed skin allergies or cases of rosacea. However, if the diagnosis is in fact cutaneous Lupus our providers can help with an effective prognosis. One of the many associated risks with having Lupus is an increased risk in developing skin cancer. This happens because of the weakened immune system. Patients who have discoid Lupus have an even greater risk of developing squamous cell carcinoma. If you have Lupus, make sure to consult with one of Pine Belt Dermatology’s providers so that we can:
- Develop an effective treatment plan for your skin.
- Find out whether or not the lupus is affecting your other organ systems.
- Provide guidance on skin care products that are less likely to irritate the Lupus rashes.
- Give tips on how to camouflage Lupus.
- Help develop skin protection that works best for your condition.
- Perform skin screenings to check for signs of skin cancer.
- Tips to Help Reduce Flare-Ups:
- Protect your skin from the sun
- Avoid tanning (indoor and outdoor)
- These habits can make Lupus much worse, and in extreme cases can lead to organ failure among Lupus patients.
- If you smoke, quit
- It has been well documented that smoking causes Lupus to worsen. It can also hinder medications taken to treat lupus rashes.
- Before taking a medicine, ask whether or not it can cause sun sensitivity
- Fit these tips into your lifestyle. They can help you avoid serious side effects from the disease such as long-term skin problems and kidney problems. If you have been diagnosed, and you follow these management tips, they can reduce your reliance on medicine to treat your condition.
The Different Types of Lupus:
Lupus panniculitis: a rash with a firm, deep, and painful growths that can infiltrate the body fat below the skin. The inflammation form this variation of Lupus will often destroy the fat cells beneath the skin. Consequently, there may be recessed and deep scarring.
Discoid Lupus: can appear as thick and scaly patches that can appear anywhere on the head (face, ears, lips, or scalp). Discoid lupus can also appear in the mouth. If this occurs, it is essential to have skin cancer screenings often. In most cases it is recommended that this screenings be done lifelong.
Subacute cutaneous Lupus: this condition can cause some people to develop a red and scaly rash that can appear on either the neck, upper back, chest, or all. The rash can sometimes form a rash that appears to be in a ring-like or bubble-like pattern. For patients that have this condition, the skin can be extremely sensitive to light. So much so that sunlight and florescent light can cause flare ups.
Acute cutaneous Lupus: this is usually characterized by the butterfly rash previously discussed, that can last for multiple days at a time.
Lupus tumidus: this Lupus rash can develop in patients who find their skin is extremely sensitive to light, specifically sunlight. The rash that ensues this reaction can appear raised and smooth.
Drug-induced Lupus: this kind of Lupus is a reaction to a certain drug that the patient may be on. This type of Lupus will typically go away once the offending drug is no longer being consumed.
So what may happen once Lupus rashes clear? The outcomes vary on a case by case basis, but some common results are spots on the skin (dark or light) and scars where the rashes once were. If either of these occur, schedule an appointment with PBD. We might be able to alleviate unwanted side effects from the disease. While there is currently no cure for Lupus, most patients are able to lead productive and healthy lives. Treatments can clear the skin and reduce the irritating symptoms so that you too may live a comfortable and active life. That is why it is so important to be sure to visit one of our clinics! For information regarding the locations and hours of operation scroll down below this page or call one of clinics (601-336-5626 for Petal or 475-9968 for Hattiesburg).
Start An Online Dermatology Visit With PBD Now!