Hidradenitis Suppurativa | FAQ
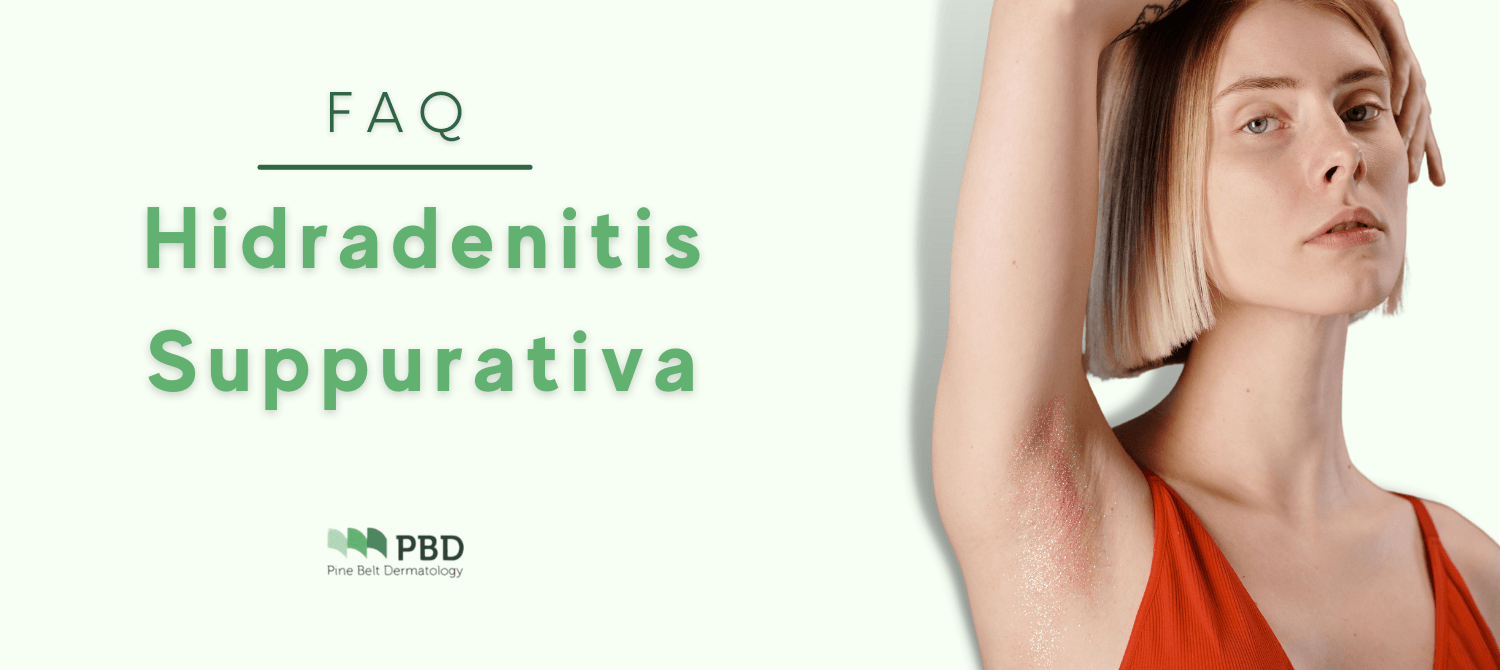
Hidradenitis suppurativa is a common skin condition that often goes unrecognized, undiagnosed, and untreated. It affects approximately 1% to 4% of the world’s population, yet we hardly know anything about it. Read on to learn more about its causes, symptoms, and possible treatments.
What Is Hidradenitis Suppurativa?
Hidradenitis suppurativa is a chronic inflammatory skin condition that begins with tiny, pea-sized bumps underneath the skin. The condition is thought to originate due to problems with the immune system. It's caused by a protein imbalance within the immune system and results in inflammation. Too many proteins within sweat glands can produce these bumps in areas where hair grows, where skin rubs together, or where sweat glands are located. Most bumps occur in places that are not easily seen, such as under the breasts, in the armpits, or in the buttocks.
Other areas where they can hide are between the thighs, which often rub together when walking and can be a major cause of skin irritation.
Causes of Hidradenitis Suppurativa
The adrenal glands that produce excess sweat also create the chemical compound known as tumor necrosis factor or TNF-alpha. This compound is an inflammatory agent that contains cytokine, which is produced by the macrophages or monocytes in your system. This type of chemical reaction is common during inflammation and can lead to other chronic skin conditions, such as apoptosis or necrosis. However, both agents are highly effective in the battle against skin cancer and other fatal diseases. The only bad news is that they can be a major source of irritation.
Are There Any Other Symptoms of Hidradenitis Suppurativa?
Hidradenitis suppurativa comes with other symptoms that most of us may not be aware of. You may experience a small area of blackheads, most of which can occur in pairs on a given patch of skin. Sometimes, these abrasions can be irritated and cause a lot of major itching, resulting in the urge to scratch that part of your skin. Scratching is a normal reaction to this condition but is still ill-advised because it will result in bleeding and scar tissue. In this case, seeking quality medical advice from a trusted physician is the best solution.
Another symptom that needs attention is the sudden appearance of tunnels. These happen on or around the area where the skin is most affected by hidradenitis suppurativa. They typically form a vast network that connects those tiny lumps and blackheads. This tunnel can be red in appearance and will emit a pungent odor when scratched or rubbed together against neighboring skin. This is often due to the collection of pus released when the skin breaks or gets irritated. Although this isn't life-threatening, you should still seek medical attention for it. It is highly treatable once it is properly diagnosed.
You should be aware that scratching an affected area can make it more prone to other infections. Germs and other toxic bacteria can enter open wounds and cause certain effects of their own. Extreme caution should be used in guarding against these and other invaders. Plus, if dirt seeps in, you could experience even greater itching due to tenderness. Washing the area with warm water and antibacterial hand soap will greatly reduce the likelihood of further issues.
What Are Some Potential Causes of Hidradenitis Suppurativa?
There is insufficient evidence as to what causes hidradenitis suppurativa. Still, there is one thing for certain: Hidradenitis suppurativa often begins when there are hair follicles that are in the part of your skin where perspiration is trapped. This happens just as the follicles are blocked by excess fluid.
Some hypotheses have developed over the years to explain this phenomenon. One is that genetics are to blame. Another is smoking, which is known to lead to premature aging of the skin and possible dryness. A third guess is hormonal imbalances of your skin's natural chemicals.
Are There Treatment Options Available for Hidradenitis Suppurativa?
Yes, there are treatment options available for those living with hidradenitis suppurativa. Some treatments may require a combination of medications and surgeries that can be used to keep your symptoms under control. Some medications may be taken orally or applied topically right to the affected area. You should do your own research and work with your doctor to determine what's right for you.
Topicals such as antibiotic creams can be used in mild cases of skin rash due to hidradenitis suppurativa. You can seek a doctor's prescription for something that's an anti-inflammatory that also prevents itching and flaking. You can get refills until you and your doctor have determined that the medication is no longer necessary. You may also opt for oral medication if the rash shows no signs of ebbing.
Medication and topical creams are considered two of the safer alternatives to surgery. They're noninvasive, and they pose limited side effects. However, there are extreme cases that only surgery can solve, such as times when the rash has become so severe that old skin may need to be removed.
What Happens After Treatment?
There is no cure for hidradenitis suppurativa, but it is a condition that is easily managed through medical and holistic measures. Good weight management is key to reducing the likelihood that skin folds will develop. Another is to keep the area clean and simply reduce stress in your life. Developing a treatment plan and complying with it is the best way to manage your condition.
Conditions like hidradenitis suppurativa and other visible skin ailments can negatively impact your self-confidence and overall well-being. However, with the right diagnosis and treatment, you can begin your journey towards healthier skin. If you would like to know more about hidradenitis suppurativa or speak to a skilled dermatologist, reach out to Pine Belt Dermatology for expert guidance.