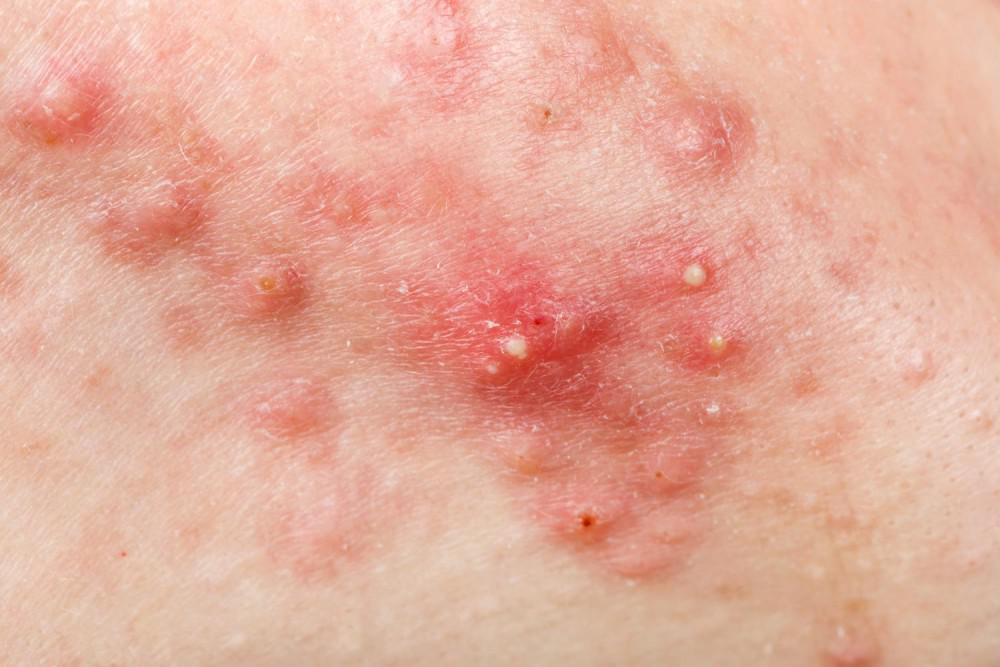
Acne woes! Most of us have been there at some point in our lives. Some of us grow out of it, some of us deal with it into adulthood. Acne is a common skin condition that affects up to 50 million American adolescents and adults. It can present as inflammatory papules (red bumps) or comedonal papules (blackheads and whiteheads). In adolescence, acne is primarily due to hormonal changes, but can also be caused by increased oil production, inflammation, and the presence of bacteria. As for adults, unfortunately the hormonal hits keep coming with acne in women being predominately related to hormones as well. The presence of acne can be found not only on the face, but also the neck, back, chest, or arms or where oil producing glands are present. Thankfully, multiple treatments exist to manage these symptoms. Disclaimer: It is important to know that all acne products can cause dryness and sensitivity, and caution should be taken if using with sensitive skin. Furthermore, many acne medications can cause sensitivity in the sun, so sunscreen and covering with hats and clothing is recommended to prevent irritation or sunburn. Now that we have that crucial piece of information out of the way, let’s talk loving your skin again.
Treatments for both inflammatory and comedonal acne consists of cleansers, topical products applied to the face and body, and also oral medications such as antibiotics or Accutane for deeper, cystic acne. Most of these medications focus on treating acne by resurfacing the skin and reducing blackheads and whiteheads or by treating the inflammatory component of acne. First line treatments involve cleansers and medications applied to the affected areas. Common cleansers contain benzoyl peroxide, an antimicrobial, or salicylic acid, a mild resurfacing agent. Both of these types of cleansers can be found over the counter. Other products that may be found over the counter can be applied topically and left on the skin and would include topical benzoyl peroxide or Differin. Differin, a type of retinoid, derived from vitamin A, also helps to resurface the skin. In the past few years, Differin has become available from a prescription only topical product, to a lower strength over the counter topical product.
Most people seeking medical help for acne have tried over the counter acne medications which either helped and stopped working, or didn’t help to begin with. As a medical provider who treats acne, the first thing I recommend is cleansing twice a day. Think of the thousands of pores on our face akin to little potholes which fill up with dirt, oil, and bacteria over the course of the day. Washing the face twice daily is a great start to an acne regimen. Also, when treating acne, I understand that busy teenagers can have compliance issues and therefore like to keep acne regimens simple. Morning and night regimens. Wash your face in the shower in the morning or night, whichever is preferred, and then at the sink when you brush your teeth the other time of the day. Unfortunately, this regimen only works if a teenager is brushing his or her teeth twice a day. Sorry moms and dads, I can only do so much.
Prescription medications to treat acne are also available and include topical antibiotics and anti-inflammatories applied to the skin. Also, in this category is a key player called Retin A. Here’s the skinny on Retin A. Retin A (also called tretinoin) may be a cream, lotion, or gel and comes in different strengths. It can be your best friend or your worst enemy in the battle against acne. When used correctly, Retin A is a wonderful medication that resurfaces the skin and is great for treating not only inflammatory acne, but also for comedonal acne. For most, the key to tolerating Retin-A relies on how you use it. I recommend to all of my patients, a slow start method when beginning Retin A. For example, on the first week, apply a pea-sized amount at bedtime 2-3 nights only such as Monday, Wednesday, and Friday. Each week, add an additional night as tolerated. Ultimately, you want to apply Retin A every night, but for some that may not be possible due to sensitivity, and that’s ok. Retin A can cause irritation and sunburn if appropriate sunscreen measures aren’t taken when outdoors.
Sometimes oral antibiotics are used in short courses to help eradicate acne bacteria and also treat inflammation associated with acne. These medications are usually in the tetracycline class and may go by the names, minocycline or doxycycline. Important take home points. Take it with food. Wear sunscreen and cover up when outdoors. You will burn. I’ve seen very bad sunburns and also blisters in patients who failed to use SPF protection when on tetracyclines.
Despite judicious use of prescription acne medications, some patients still may not have an adequate response to therapy. For those people who suffer from chronic nodulocystic acne, another medication known as Accutane may be an option. This medication is basically an oral form of Retin A. A thorough medical history must be taken prior to deciding to pursue Accutane. Treatment with Accutane also requires an average of 6 months of therapy including regular lab testing and monthly office visits with your dermatologist. I like to save Accutane as my heavy hitter when treating acne and use it when conventional methods fail. If my patient is a candidate for this specific type of treatment, it is a game changer for sure.
With adult acne, treatment regimens are similar, however an additional medication called spironolactone may be used for women suffering from what I like to affectionately call, “grown-up acne”. As women age, our hormones do wonky things and fluctuations in our hormones trigger surges of grown-up acne. Spironolactone is an oral medicine that blocks the testosterone cause of acne in women. For patients who are healthy, a simple blood test to assess kidney function and electrolytes is performed and this may be an option to reduce acne breakouts.
In conclusion, acne can be frustrating for patients and for the parents of patients. The good news is that today’s treatments are easily accessible with first-line therapy being available over the counter. For those who need a little more, I recommend talking to your dermatologist for further options in treating this common but mendable skin condition.